Physical Therapy Services
Could Pelvic Floor Dysfunction Treatment Physical Therapy be the Answer?
Women’s health is a specialty of physical therapy that is often geared towards addressing the dysfunction of the pelvic floor. Pelvic floor dysfunction is the inability to control the muscles of your pelvic floor. You may benefit from women’s health physical therapy if you have diagnoses such as prolapse, urinary incontinence, dyspareunia, vaginismus, vestibulitis, vulvodynia, coccyx pain, piriformis syndrome, sciatica, pelvic pain/dysfunction, constipation, fecal incontinence, and lower abdominal pain.
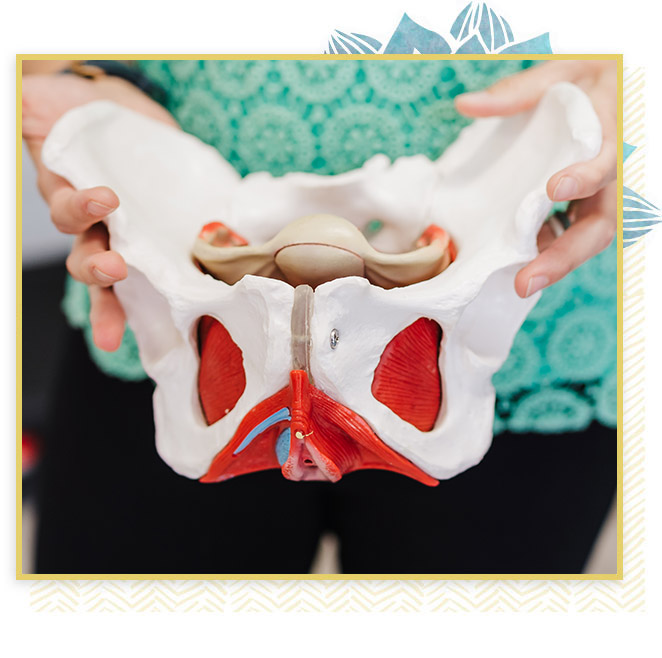
The pelvic floor includes all the muscles, ligaments, nerves, and connective tissue that stretch across the pelvis. It's not just a clever name; the pelvic floor is actually the floor of your pelvis. Muscles there wrap from the tailbone and across the bony pelvis. It's an incredibly important area, connecting the upper and lower body. Pelvic Floor Dysfunction Treatment Physical Therapy aims to correct problems.
Underactive pelvic floor
Sometimes the muscles of the pelvic floor are underactive or weakened, resulting in pelvic organ prolapse and fecal and/or urinary incontinence. Symptoms of a weakened pelvic floor may include leaking small amounts of urine when coughing, sneezing, laughing or running, or failing to reach the toilet in time.
Overactive pelvic floor
Sometimes the muscles of the pelvic floor are overactive or have increased tone, leading to an inability of the pelvic floor muscles to relax. Symptoms may include increased urge to urinate, painful urination, constipation or bowel strains, pain in the pelvic region, and discomfort during sexual intercourse.

Pregnancy and Postpartum
According to experts in a 2014 article in the Journal of Sports Physical Therapy, “anywhere from 24% to 90% of women experience low back or pelvic-region pain when they are pregnant.” More than a third of women still have pain 1 year after giving birth. The ability of a woman’s body to carry and deliver a baby is truly amazing and sacred. During pregnancy, a woman’s body undergoes many hormonal, musculoskeletal, and postural changes that can contribute to pain. As the baby grows and more load is placed on the pelvic floor, increased symptoms of incontinence can occur. In the postpartum phase, women need adequate time to heal from the delivery process, which is very individualized with every woman. External demands and loads, such as caring for older siblings and carrying car seats, are additionally placed on the mother. Some women may experience diastasis recti, or separation of the abdominal wall, which may impact how and when they may return to physical activity postpartum.
Running and Orthopedics
Running is a great form of exercise, and just like any other sport, it can put stress and strain on your body. If you consider yourself a runner, the last thing you want is for an injury to keep you from running. If an injury occurs, you’ll want to get back on your feet as fast as possible. Resilience PT is dedicated to helping women run with innovative practices that help runners increase speed, recover from and avoid injury. Our therapy specializes in running performance enhancement and injury evaluation and management. The holistic approach we use looks into both running gait analysis and treatment intervention. Our highly skilled specialists conduct in-depth evaluations to determine the best treatment according to what makes you unique.

Treatments
IASTM
Instrument Assisted Soft Tissue Mobilization (IASTM) is a process in which the clinician uses a set of hand held instruments to break down the scar tissue and fascial restrictions in soft tissues (muscles, ligaments, tendons, fascia, and nerves). This can be useful to address tight tissue following a C-section, or to mobilize tight muscles during and following pregnancy.
Trigger Point Dry Needling
Intramuscular trigger point dry needling is an evidence-based treatment that targets tight points within a muscle which may cause pain and limit mobility. Muscular trigger points can cause dysfunction locally at the muscle site, or refer pain to other points in the body. Dry needling treatment relieves abnormal muscle tightness or spasm, and can allow fairly immediate pain relief.
Education
Education is such a vital component of the rehab process. You will be given a home program at the end of each treatment session that may be modified throughout the course of treatment and individualized to your specific needs. You will learn a lot about how your body works, what “normal” function is, and how you can help yourself get better.
Pelvic Floor Relaxation / Downtraining the Nervous System
The nervous system can be thought of as two main branches: sympathetic (“fight or flight” - stress) and parasympathetic (“rest and digest” - calm). Sometimes you need your “fight of flight” to be turned on, but when it’s turned on constantly, it can lead to increased pain, anxiety, tension, sensitivity, bowel problems, autoimmune reactions, inflammation, and disturbed sleep. It is not healthy to be in this constant “red-alert” state for long periods of time. Often we have to remind our bodies to turn on the relaxation system. This is often done through re-training our bodies how to breathe correctly. With each breath, the diaphragm drops down and allow the pelvic floor to lengthen.
Biofeedback
Biofeedback is a training technique that assists the patient in gaining voluntary control over muscular or autonomic nervous system functions. Biofeedback is often a useful adjunct to pelvic floor muscle training. Surface EMG is a form of biofeedback that uses surface electrodes to measure electrical activity of a muscle contraction, and produces either auditory or visual feedback in response to the muscle activity. Diagnoses to consider for biofeedback training include: stress and urge urinary incontinence, bowel incontinence and constipation, and pelvic pain.
DNS
Dynamic Neuromuscular Stabilization (DNS) is an assessment and treatment approach founded on neurodevelopmental movement patterns that we establish within the first years of life. We use these foundational movement patterns to restore dysfunctions that can result in injury.
Cupping
Cupping is a technique used to decrease pain and muscle tension and improve blood flow and tissue repair. Cups are placed over a target area and a negative pressure is created, forming a suction to the skin. Different forms of cupping exist with a variety of cup types and suction techniques.
Pelvic Floor Muscle Training
The goal of pelvic floor muscle training is to improve the functional condition of the pelvic floor. The focus of pelvic muscle training may be strength training, endurance training, or coordination training depending on the specific needs of the patient.